Urine casts are cylindrical, cigar-shaped structures produced by the kidney and present in the urine in certain disease conditions.
All casts are composed of a mucoprotein known as Tamm-Horsfall protein which is secreted by the distal loop of Henle, the distal tubule and the collecting ducts at a fairly constant rate. A significant number of urinary casts usually indicates the presence of renal disease.
Formation of Casts
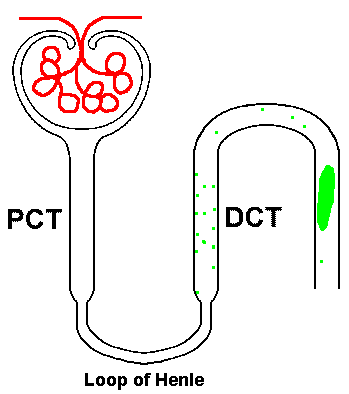
Urinary casts are formed only in the distal convoluted tubule (DCT) or the collecting duct. The proximal convoluted tubule (PCT) and loop of Henle are not locations for cast formation. Casts are the result of solidification of material (protein) in the lumen of the kidney tubules.
Once formed, these casts of the tubule are eliminated via the urine and may be seen in the urine sediment. They may contain RBCs, WBCs, renal epithelial cells, fat globules, bacteria, and degenerated forms of any of these structures, which are seen as granules.
Aggregates of plasma proteins, including fibrinogen, immune complexes, and globulins, may also be seen as granules within a cast.
Types of urinary Casts
Urinary casts can be divided into two main categories : Acellular and Cellular Casts.
| Acellular Casts | Cellular Casts |
|---|---|
| Hyaline Casts | Red Blood Cell Casts |
| Granular Casts | White Blood Cell Casts |
| Waxy Casts | Bacterial Casts |
| Fatty Casts | Epithelial Cell Casts |
Acellular Casts
Hyaline Casts
Hyaline casts are the most common type of casts which are composed of solidified Tamm-Horsfall mucoprotein. They have smooth texture and a refractive index very close to that of the surrounding fluid.
Generally, hyaline casts have parallel sides with clear margins and blunted ends. Hyaline casts can be seen even in healthy patients. They may be seen in increased numbers during dehydration, exercise or diuretic medicines.
Granular Casts
Granular casts result either from the degeneration of cellular casts, or direct aggregation of plasma proteins or immunoglobulin light chains. They have a textured appearance which ranges from fine to coarse in character.
Their appearance is generally more cigar-shaped and of a higher refractive index than hyaline casts. They are seen after sternous exercise, chronic renal diseases, acute tubular necrosis etc.
Waxy Casts
Waxy casts represent the final stage of degeneration of cellular casts. They are more refractile and therefore easier to see compared to hyaline casts.
They are uaually seen in tubular injury of a more chronic nature than granular or cellular casts like severe chronic renal disease and renal amyloidosis. These casts are also called renal failure casts.
Fatty Casts
Fatty casts are formed by the breakdown of lipid-rich epithelial cells. These contain lipid droplets within the protein matrix of the cast and are identified by the presence of refractile lipid droplets. They are usually seen in the conditions like tubular degeneration, nephrotic syndrome, hypothyroidism etc.
Cellular Casts
A cellular cast may be composed of any of the cells found in the urine sediment, such as RBC, WBC, or renal tubular epithelial cell. The cellular cast appears to result from a clumping of cells that are incorporated in a protein matrix.
Red Blood Cell Casts
Red blood cells may stick together and form red blood cell casts. Such casts are indicative of glomerulonephritis, with leakage of RBC’s from glomeruli, or severe tubular damage.
White Blood Cell Casts
White blood cells (generally neutrophils) are present within or upon casts. These casts are typical for acute pyelonephritis, but they may also be present with glomerulonephritis.
They may also be seen in acute interstitial nephritis, lupus nephritis, and acute papillary necrosis.
Renal Tubular Epithelial Cell Casts
These casts are composed of renal epithelial cells. These casts are seen in conditions such as renal tubular necrosis, viral disease (such as CMV nephritis), and kidney transplant rejection.
Bacterial Cell Casts
Bacterial casts are casts composed of bacteria in a protein(hyaline) matrix. Bacterial casts are diagnostic of acute pyelonephritis or intrinsic renal infection.
Summary
| Casts | Composition | Associated Conditions |
|---|---|---|
| Hyaline casts | Solidified Tamm-Horsfall mucoprotein | Normal individualsDehydrationHeavy exercise |
| Granular casts | Various cell types (Degeneration of cellular casts, Aggregates of plasma proteins or immunoglobulin light chains) | After sternous exerciseChronic renal diseasesAcute tubular necrosis |
| Waxy casts (renal failure casts) | Various cell types (Final stage of degeneration of cellular cast) | Severe chronic renal diseaserenal amyloidosis |
| Fatty casts | Lipid droplets within the protein matrix of the cast | Tubular degenerationNephrotic syndromeHypothyroidism |
| RBC Casts | Red Blood Cells | PyelonephritisGlomerulonephritisAcute interstitial nephritisLupus nephritis |
| WBC Casts | White Blood Cells | Glomerulonephritis |
| Epithelial Cell Casts | Renal Tubular Epithelial Cells | Renal tubular necrosisViral DiseasesKidney transplant rejection |
| Bacterial Cell Casts | Bacterial Cells | Acute pyelonephritisIntrinsic renal infection |
Frequently asked Questions
Q 1. What does it mean to have cast in your urine?
Q 2. Are casts in urine normal?
Q 3. What causes granular casts in urine?
Q 4. What is the normal range for casts in urine?
Q 5. What do red blood cell casts in the urine always indicate?
Q 6. What do crystals in urine indicate?
Q 7. How are casts formed?
Q 8. Why is there mucus in my urine?
Q 9. What is damaging to kidneys?
Q 10. What causes the protein in the urine?
– High protein diet.
– Stress.
– Pregnancy.
– Strenuous exercise.
If the protein in the urine is abnormally high, the doctor will request additional urinalysis and other necessary tests to find out the culprit.
Q 11. What should not be found in urine?
1. Nitrites
2. Hemoglobin
3. Glucose
4. Protein
5. Ketones
6. Bilirubin
7. Red blood cells
8. White blood cells
Q 12. How do you get rid of crystals in your urine?
Percutaneous nephrolithotomy
Ureteroscopy – a thin scope with a camera on the end is passed through the bladder to access the kidneys.
Extracorpeal shock wave lithotripsy – delivering sound waves to break the stone into tiny pieces making them easy to eliminate from the body.
Q 13. Can dehydration cause crystals in urine?
Q 14. When your urine is tasteless?
Q 15. What are the four major reasons a urinalysis may be done?
– Routine medical exam to screen or detect early signs of an underlying medical condition.
– Check for the presence of blood in the urine.
– To diagnose urinary tract infection.
– To note if you have any signs of kidney-related diseases, diabetes, and to monitor the progress of treatment for such conditions.
Q 16. What indicates kidney infection in a urine test?
Q 17. Are eggs high in oxalate?
Q 18. What are the worst foods for kidney stones?
1. Chocolates
2. Beets
3. Spinach
4. Tea
5. Rhubarb
6. Nuts
These foods are rich in oxalate which increases the possibility of developing kidney stones.
Q 19. Is broccoli high in oxalate?
Q 20. What do crystals in urine look like?
Q 21. What foods help repair kidneys?
1. Cabbage
2. Red bell peppers
3. Onions and garlic
4. Apples
5. Berries, especially blueberries and cranberries



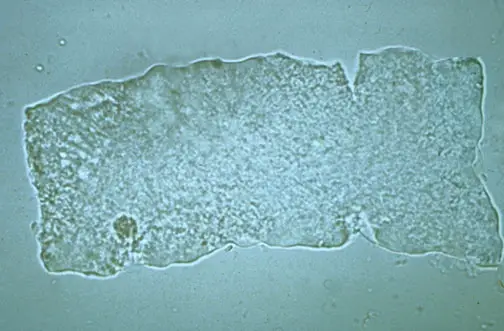
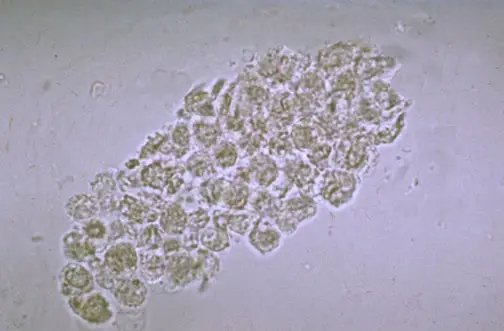
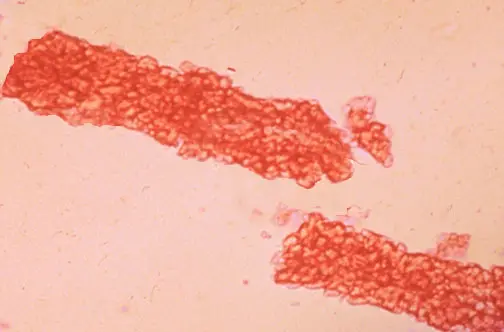

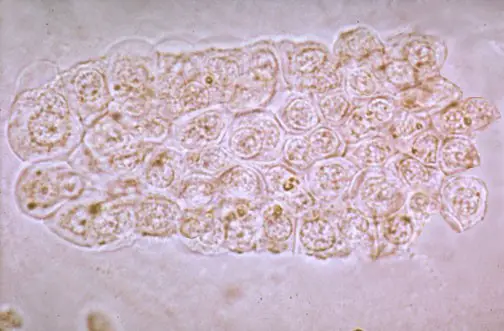
These r rare conditions n not seen usually.
Best photography best interpretation well done
real interesting under microscope,credit!
Thanks for these pictures. Will be helpful in training.
we always encounter these casts and helped a lot. Thanks
Am 24 years of age and when ever are urinate , the urine passout in parallel for almost 1 year today ,thank you .
Good to see various types of cast with definition
Really helpfu, Thanks
GOOD WORK THANKS
in the summary table the condition associated with RBC and WBC cast is switched